What is a Colonoscopy?
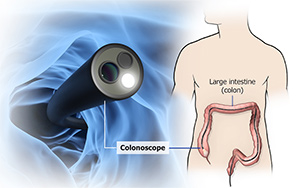
A colonoscopy is a medical procedure used to examine the inside of the large intestine (colon) and rectum. It is performed by a gastroenterologist, using a thin, flexible tube called a colonoscope. The colonoscope has a light and a small camera attached to its tip, which allows the doctor to see images of the colon lining on a screen in real time.
Who is Suitable for a Colonoscopy?
Colonoscopy is recommended for a wide range of individuals as a routine screening measure or to investigate symptoms. People who may benefit from a colonoscopy include:
- Individuals with a family history of colorectal cancer or certain types of polyps
- People experiencing digestive symptoms such as persistent abdominal pain, rectal bleeding, changes in bowel habits (diarrhoea or constipation), or unexplained weight loss
- Patients with a history of inflammatory bowel disease (IBD), such as Crohn’s disease or ulcerative colitis
- Those who have previously had polyps or colorectal cancer and require surveillance
Your doctor will assess your medical history, risk factors, and current symptoms to determine if a colonoscopy is the right test for you. In some cases, screening may begin earlier, especially if you're under 45 and have symptoms or a family history.
Benefits of Colonoscopy
Colonoscopy is one of the most reliable methods for evaluating the colon and rectum. Its benefits include:
- Early detection of colorectal cancer, which can greatly improve treatment success and survival rates
- Removal of precancerous polyps during the procedure, helping to prevent cancer from developing
- Direct visualisation of the entire colon, offering a complete assessment
- The ability to diagnose a variety of conditions such as diverticulosis, IBD, and bleeding sources
- Biopsy capability, which allows doctors to collect samples for further testing without requiring additional procedures
Types of Colonoscopy
Depending on the purpose and method, there are a few types of colonoscopy. Your doctor will recommend the most appropriate type for your situation.
- Diagnostic colonoscopy: This is used to investigate symptoms such as bleeding, unexplained weight loss, or persistent abdominal pain. It helps determine the cause of your symptoms and confirm a diagnosis.
- Screening colonoscopy: This is done in individuals without symptoms but with risk factors such as age or family history. It is used to detect early signs of colorectal cancer or polyps.
- Surveillance colonoscopy: If you’ve had polyps, cancer, or inflammatory bowel disease in the past, this type is used for regular follow-up to monitor for recurrence or new changes.
- Therapeutic colonoscopy: This is performed to diagnose and treat conditions. It can include removing polyps, stopping bleeding, or dilating narrowed areas of the colon.
All these types use the same basic technique, but the reason for the procedure may differ. In every case, the colon must be prepared in advance by following a bowel cleansing process to ensure clear visibility during the examination.
What to do Before a Colonoscopy?
Preparing for a colonoscopy is an important part of the process to ensure your doctor can clearly see the inside of your colon. A clean colon allows for a more accurate and successful examination.
Your doctor will give you specific instructions before your procedure, which typically include:
- Dietary changes: A few days before your colonoscopy, you may be asked to follow a low-fibre or clear liquid diet. Only clear fluids such as water, broth, apple juice, and sports drinks are allowed the day before the procedure.
- Bowel preparation: You must drink a special laxative solution that helps empty your bowels. This is usually done the evening before the procedure and may be split into two doses for better results.
- Medication review: Inform your doctor of all your medications and supplements. You may be asked to stop certain drugs, such as blood thinners, for a short period before the colonoscopy.
- Arrange transport: Since sedation is usually given, you will need someone to take you home after the procedure.
Following the instructions carefully is important. If your colon isn’t fully clean, the procedure may need to be rescheduled or repeated.
What Happens During a Colonoscopy?
When you arrive at the clinic or hospital, you will be asked to change into a gown and lie on your side, usually with your knees drawn toward your chest.
Here is what typically happens:
- Sedation: You will be given a light (“twilight”) anaesthetic to make you drowsy and relaxed. You are unlikely to be aware of the procedure and may not remember anything about the procedure.
- Insertion of colonoscope: The doctor will gently insert the colonoscope into your rectum and slowly guide it through the colon. Air or carbon dioxide is introduced to inflate the colon slightly and improve visibility.
- Examination: As the scope moves through the colon, the doctor looks for polyps, inflammation, bleeding, or other abnormalities.
- Polyp removal or biopsy (if needed): Small polyps can be removed during the same session. If there are areas that need further examination, a small tissue sample (biopsy) may be taken.
- Completion: The colonoscope is slowly withdrawn, and the procedure usually takes between 20 to 45 minutes.
You will be monitored after the procedure as the sedation wears off, which may take about an hour.
What to Expect After a Colonoscopy?
After the procedure, most patients feel fine, although it’s normal to feel slightly bloated or have mild cramping due to the air introduced into the colon.
Here’s what to expect:
- Recovery from sedation: You’ll be observed in the recovery area until you are awake and alert. You should not drive, operate machinery, or make important decisions for the rest of the day.
- Passing gas: You may pass gas for a few hours after the procedure, which helps relieve bloating.
- Resuming diet: You can usually resume eating once you're fully awake unless your doctor advises otherwise. Start with light meals at first.
- Results: If polyps were removed or biopsies taken, results may take a few days. Your doctor will explain any findings and discuss the next steps if needed.
- Mild discomfort: You might experience a small amount of blood in your stool if a biopsy or polyp removal was performed, but this should go away quickly.
Contact your doctor if you experience severe abdominal pain, fever, or persistent bleeding.
Early detection is key
Colonoscopy is an excellent tool for early detection and treatment of a wide variety of colonic diseases. If polyps are removed early, the risk of developing colorectal cancer is significantly reduced. When colorectal cancer is caught in its early stages, treatment is more likely to be successful.
In cases where no issues are found, your doctor will recommend when you should return for your next screening, often in 5 to 10 years. If certain findings are present, such as large or multiple polyps, follow-up may be required.
Regular screening and timely follow-ups offer the best outcomes for long-term digestive health.
Colonoscopy Risks
Colonoscopy is generally safe, but like any medical procedure, it carries some risks. These are rare and often mild, but being informed is good.
Possible risks include:
- Bleeding: Especially if a polyp is removed or a biopsy is taken. Most cases are minor and stop on their own.
- Perforation: A small colon wall tear may occur in rare cases. This might require surgical repair.
- Reaction to sedation: Some people may experience nausea, low blood pressure, or allergic reactions to the sedative.
- Infection: While uncommon, there is a slight risk of infection from tissue removal.
Your doctor will explain all potential risks before the procedure and ensure safety measures are in place.
What if a Colonoscopy is Delayed?
Delaying a colonoscopy can impact your health, especially if you are at risk for colorectal cancer or have ongoing symptoms. Early-stage colon cancer often has no noticeable symptoms, so delays in screening could mean missing the chance to detect and treat it early.
Other consequences of delay may include:
- Worsening of symptoms or underlying conditions
- Missed opportunity to remove polyps before they turn cancerous
- Delayed diagnosis of conditions like inflammatory bowel disease or diverticulitis
If you’ve been advised to undergo a colonoscopy and are hesitant or unable to schedule it immediately, speak with your doctor. They can help address concerns, offer alternative timelines, or explore other options if necessary.

